How Are Allergies and Asthma Connected?
Allergy and asthma are closely linked, as allergic reactions often trigger asthma symptoms in sensitive individuals. When a person with asthma is exposed to allergens such as pollen, dust mites, or pet dander, their immune system responds by inflaming the airways, which can lead to difficulty breathing, coughing, and wheezing. Dr. Jon E. Stahlman, MD, at Allergy & Asthma Center, stresses the importance of diagnosing and treating both conditions together. For more information, please contact us or book an appointment online. We have convenient locations to serve you in Lawrenceville GA, Atlanta GA, and Conyers GA.
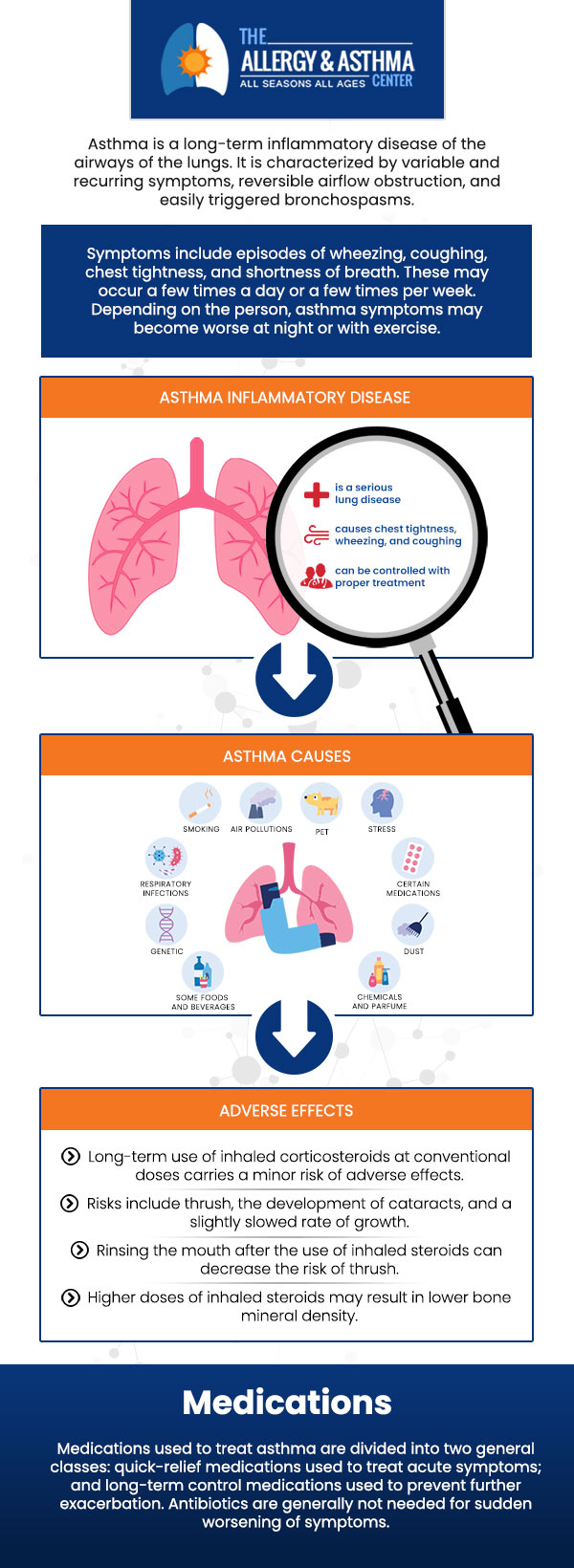
Table of Contents:
What is allergic asthma, and how does it develop?
Can treating allergies help control asthma?
Is asthma more common in people with eczema or hay fever?
How does Dr. Jon E. Stahlman test if asthma is allergy-related?
Allergic asthma is a type of asthma triggered by allergens such as pollen, dust mites, mold, or pet dander. It occurs when the immune system overreacts to these allergens, causing inflammation and narrowing of the airways. This inflammation makes it harder to breathe and leads to symptoms like wheezing, coughing, shortness of breath, and chest tightness. Allergic asthma is one of the most common forms of asthma, especially in individuals with a family history of allergies or asthma.
The development of allergic asthma is typically gradual. It begins when the body’s immune system mistakenly identifies harmless substances as harmful. Upon exposure to an allergen, the immune system produces antibodies called immunoglobulin E (IgE). These antibodies trigger the release of chemicals such as histamine, which cause the symptoms of an allergic reaction, including airway inflammation. Over time, repeated exposure to allergens can lead to chronic inflammation and permanent narrowing of the airways, worsening asthma symptoms.
At the Allergy & Asthma Center, our team helps patients understand the relationship between allergies and asthma. They work to identify specific allergens that may trigger asthma attacks and to develop effective treatment plans to manage symptoms. This might include medications, lifestyle changes, or immunotherapy to reduce sensitivity to allergens and improve asthma control.
Yes, treating allergies can help control asthma, especially when allergic reactions are a primary trigger for asthma symptoms. For many people, exposure to allergens can trigger an asthma attack by causing the airways to become inflamed and constricted. Managing allergies effectively can reduce this inflammation, leading to fewer asthma symptoms and less reliance on asthma medications.
Treatments for allergies, such as antihistamines, nasal sprays, and immunotherapy, can help reduce the body’s sensitivity to allergens. Immunotherapy, in particular, has been shown to provide long-term relief by gradually desensitizing the immune system to specific allergens. By addressing the underlying allergic response, immunotherapy can reduce the frequency and severity of asthma attacks.
In addition to medications, patients at the Allergy & Asthma Center are often advised to implement lifestyle changes to avoid allergens whenever possible. This might include using air purifiers, cleaning homes regularly, and avoiding outdoor activities during peak pollen seasons. For patients with asthma and allergies, a combination of allergy treatments and asthma management strategies can result in better control over both conditions.
By treating allergies, individuals with allergic asthma can improve their quality of life, experience fewer asthma flare-ups, and reduce the need for emergency treatments. Our expert team at the Allergy & Asthma Center tailor treatment plans to each patient’s unique needs, aiming for comprehensive control of asthma and allergies.
Yes, asthma is more common in people with both eczema (atopic dermatitis) and hay fever (allergic rhinitis). These conditions are all part of a group of allergic diseases known as atopic diseases, which are characterized by an overactive immune system response to allergens. Research shows that individuals with eczema or hay fever are more likely to develop asthma, especially if they have a family history of allergies or asthma.
Eczema, a chronic skin condition characterized by itchy, inflamed skin, often appears in early childhood and is frequently associated with other allergic conditions like hay fever and asthma. People with eczema have an increased risk of developing hay fever, and in turn, those with hay fever are at a higher risk of developing asthma. This progression is sometimes referred to as the “atopic march,” where one allergic condition leads to another over time.
Hay fever, or allergic rhinitis, is another condition that can increase the risk of asthma. People with hay fever often have chronic inflammation of the nasal passages due to exposure to allergens like pollen, dust mites, or mold. This nasal inflammation can contribute to airway inflammation, which may eventually lead to asthma.
At the Allergy & Asthma Center, our team focuses on diagnosing and treating all aspects of atopic diseases. Managing eczema or hay fever, they can help prevent the development of asthma and improve overall quality of life. Early intervention and effective management of allergic conditions are key to reducing the risk of asthma in individuals with eczema or hay fever.
Dr. Jon E. Stahlman, MD, at the Allergy & Asthma Center, uses a comprehensive approach to test if asthma is allergy-related. The first step involves a thorough medical history and physical examination to assess the patient’s asthma symptoms, triggers, and any history of allergic conditions like hay fever, eczema, or family members with asthma or allergies.
Once a history is established, Dr. Stahlman may recommend specific allergy tests to identify potential triggers of asthma symptoms. One common test is the skin prick test, which involves placing small amounts of allergens on the skin and then pricking the skin’s surface to allow the allergens to enter. If the patient is allergic to a particular substance, a small raised bump or welt will appear at the test site. This test is useful for identifying allergens such as pollen, pet dander, mold, and dust mites.
Another test used to determine if asthma is allergy-related is blood testing for specific IgE antibodies. This test measures the level of IgE in the blood, which is produced by the immune system in response to allergens. Elevated IgE levels suggest an allergic response, and the test can help identify the specific allergens that may be triggering asthma symptoms. In some cases, Dr. Stahlman may also perform pulmonary function tests (PFTs) to assess the overall function of the lungs and determine the extent of airway obstruction. If asthma is found to be allergy-related, treatment plans can be developed that may include medications, lifestyle changes, or immunotherapy to manage both asthma and allergies effectively. For more information, please contact us or book an appointment online. We have convenient locations to serve you in Lawrenceville GA, Atlanta GA, and Conyers GA.We serve patients from Lawrenceville GA, Atlanta GA, Conyers GA, Scottdale GA, Tucker GA, Rock Chapel Rd GA, Klondike Rd GA, Suwanee GA, Moon Place Rd GA and Dacula GA.

Additional Allergy & Asthma Services
▸ Allergy Shots
▸ Allergy Testing
▸ Asthma
▸ Bronchodilators
▸ Drug Allergy
▸ Food Allergy
▸ Insect Allergy
▸ Nasal/Sinus Allergies
▸ Pediatric Allergy
▸ Pediatric Asthma
▸ Skin Allergy
▸ Spring Allergies