Asthma Treatment Questions and Answers
Are you looking for Asthma Treatment? Look no further and come to The Allergy & Asthma Center! We evaluate each patient individually to determine the triggers of an asthma attack and create the best treatment for that patient. For more information, please contact us or book an appointment online. We serve patients from Lawrenceville GA, Atlanta GA, Conyers GA, Suwanee GA, Duluth GA, Grayson GA, Decatur GA, Brookhaven GA, Lithonia GA and Covington GA.
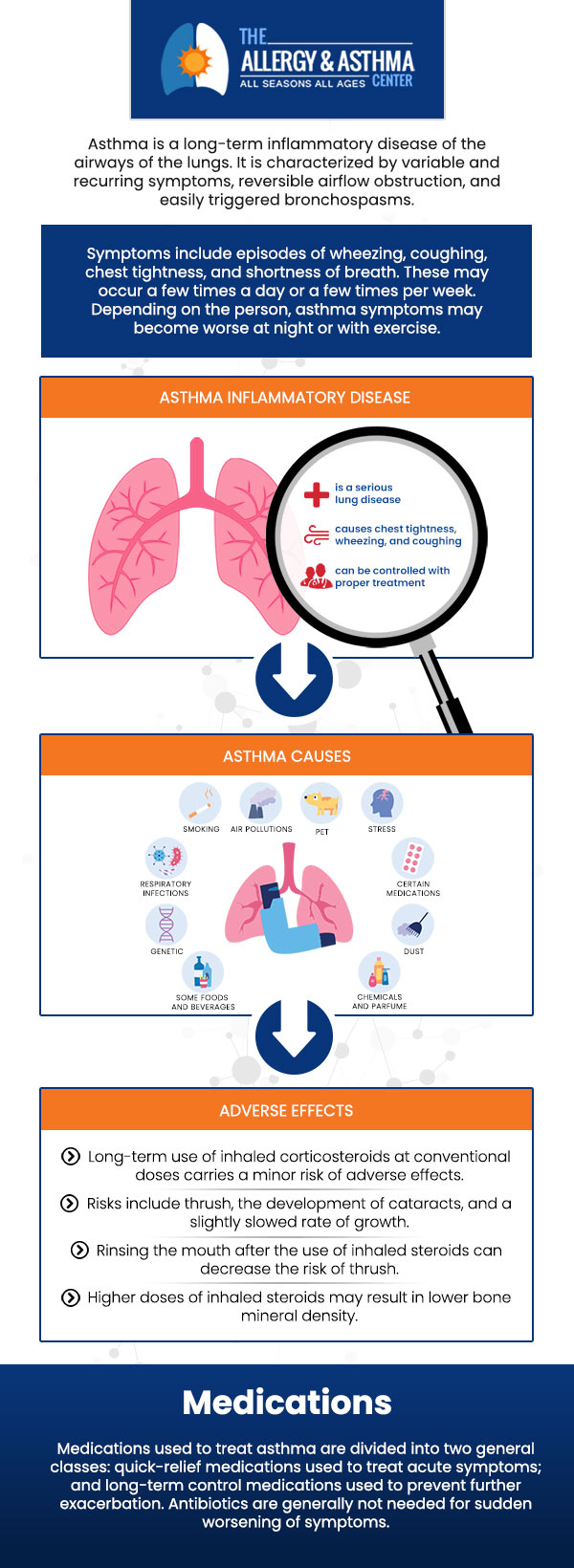


Table of Contents:
What Is Asthma?
What Are The Symptoms of Asthma?
What Triggers Asthma Symptoms?
How is Asthma Diagnosed?
How Is Asthma Treated?
The word asthma is derived from Greek and is literally translated as “panting” or “short drawn breath”. If you or your child has ever experienced an asthma attack, this translation seems quite appropriate. Yet asthma specialists are quick to point out that most asthma patients have more subtle symptoms and, only rarely, experience asthma “attacks”.
Asthma symptoms result from hyper-responsiveness of the lungs to allergic and non-allergic triggers. This hyper-responsiveness leads to two main processes within the lungs causing asthma symptoms. One is airway inflammation in the smaller bronchial tubes. This inflammation causes swelling and increased mucus production which narrows the airways. The second process is bronchial constriction. This is when the muscles around the bronchial tubes tighten and squeeze the airways. Both of these processes– the swelling and mucous production inside the tubes and the muscular tightening on the outside of the tubes – lead to airway obstruction, with subsequent wheezing, cough, tightness in the chest, and difficulty breathing.
However, it is extremely important to recognize that all asthmatic patients have the same symptoms and severity can vary. Patients with mild asthma, especially children, may present with a cough, and no other symptoms. The presenting symptoms can vary from prolonged coughing with a cold to severe breathing difficulties requiring hospitalizations.
The airways of asthma patients tend to be highly reactive to a variety of triggers, both allergic and non-allergic. Allergies are one of the primary causes of asthma symptoms, especially in children. Common allergic triggers of asthma include dust mites, mold and mildew, pet dander, feathers, cockroaches, as well as weed, tree, and grass pollen.
The response to allergens can be immediate (within minutes to hours) but some patients can have a slow build up of symptoms over days to weeks. Approximately one half of all asthmatics have non-allergic asthma, i.e., their symptoms are brought on not by allergens, but by exposure to non-allergic triggers, or irritants. The classic non-allergic triggers would include: an upper respiratory viral infections (the common cold), exercise, laughter, cold air, exposure to cigarette smoke and other strong smells (perfumes, aerosols, cleaning products, etc.), and changes in the weather.
Asthma is diagnosed through a combination of detailed history of asthma symptoms as well as lung function testing (spirometry) in older children and adults. Spirometry is a simple breathing test that measures how much and how fast air you can blow air out of your lungs. Sometimes spirometry is done before and after a short acting asthma medicine (bronchodilator) is inhaled. The diagnosis of asthma in infants and young children can be especially challenging, due to the fact that lung function testing in young children is difficult. Commonly, infants and young children are often diagnosed with “reactive airways disease” (RAD) when symptoms occur with URIs (colds) which may eventually be confirmed as asthma over time. A strong family history may lead doctors to diagnose asthma at an earlier age. Since allergies play a large role in asthma, allergy testing will be indicated in many cases to identify triggers. Your physician may also ask about other conditions that can worsen asthma, such as chronic sinus infections and gastroesophageal reflux (heartburn).
Allergy and asthma specialist should be actively involved in formulating a comprehensive program to best manage your asthma. Depending on several factors, such as the frequently and severity of symptoms and measurement of lung function, your asthma specialist will decide which medicines are needed.
Controller Medications: are usually prescribed for patients who have asthma symptoms consistently at least two or three days per week. Patients who require rescue medication to control night time cough or daily shortness of breath are commonly placed on these preventative medications.
Inhaled Corticosteroids: are the first-line treatment of persistent asthma and are the most commonly prescribed controller medications. These medications are inhaled one to two times daily to decrease airway inflammation and reduce the frequency of asthma symptoms. They need to be used consistently on a daily basis in order to be effective. They are NOT to be used to treat an acute or sudden attack of symptoms. They have an excellent safety profile and are appropriate even for young children and senior citizens. Often they are combined with long-acting bronchodilators (LABAs) to help provide control of more moderate to severe asthma.
Leukotriene inhibitors: are another type of controller medication. Leukotriene inhibitors come in tablets, chewables, or dissolvable powder. It is often prescribed as an add on medication along with inhaled corticosteroids to improve asthma control or by itself in cases of very mild asthma.
Biologic Therapies: Biologics are the newest asthma therapies. These injectable asthma medications (omalizumab, dupilumab, mepolizumab, benralizumab, reslizumab to name a few) target specific molecules involved in the asthma inflammatory process. These treatments are specific for certain types of asthma. Omalizumab is used to treat asthma triggered by allergies whereas the other biologic drugs are used to treat asthma in patients with a large amount white blood cells called eosinophils. Biologic medications are used as controller medications to treat severe asthma that has not been responded to maximum doses of other controllers such as inhaled corticosteroids, long-acting bronchodilators and leukotriene inhibitors.
Older asthma medications such as theophylline, cromolyn, nedocromil are also used as controllers but much less commonly.
Rescue Medications:
Bronchodilators: Rescue medications, often referred to as bronchodilators, are designed to provide immediate relief of bronchial constriction. Examples of these medications include albuterol, xopenex, and ipratropium. They may be given as inhalers or aerosolized to be used in a nebulizer.
Oral or Injectable Steroids: Oral or injectable steroids are often prescribed to rapidly reduce the airway inflammation during acute or chronic asthma. Short courses of corticosteroids are generally safe if taken infrequently but can cause side effects if used for long periods of time or too frequently. Taking preventative medicines regularly can reduce the need for oral and injectable steroids.
Immunotherapy (allergy shots): An allergy and asthma specialist may recommend immunotherapy therapy for patients who have difficulty controlling their allergies and/or asthma. Immunotherapy works by making the immune system more tolerant to allergens and thus decreasing the hyper responsiveness of the airway to allergens in the environment. Studies suggest that immunotherapy can also be effective in preventing an allergic individual from developing asthma.
Finally, a team approach with your physician may include an asthma action plan. Your doctor may give you a list of symptoms with corresponding recommendations about when to start medications, or when to seek medical attention. Your board certified allergist is the best resource for helping decide if any of these therapies are best for you or your child.

Additional Allergy & Asthma Services
▸ Allergy Shots
▸ Allergy Testing
▸ Asthma
▸ Bronchodilators
▸ Drug Allergy
▸ Food Allergy
▸ Insect Allergy
▸ Nasal/Sinus Allergies
▸ Pediatric Allergy
▸ Pediatric Asthma
▸ Skin Allergy
▸ Spring Allergies